MENU
Browse around
topics
Hey there!
Integrative nurse practitioner, lactation specialist & women's health advocate.
I'm Ariella
Integrative primary care and advanced lactation support

Post Title Here
Category
Post Title Here
Category

Post Title Here
Category
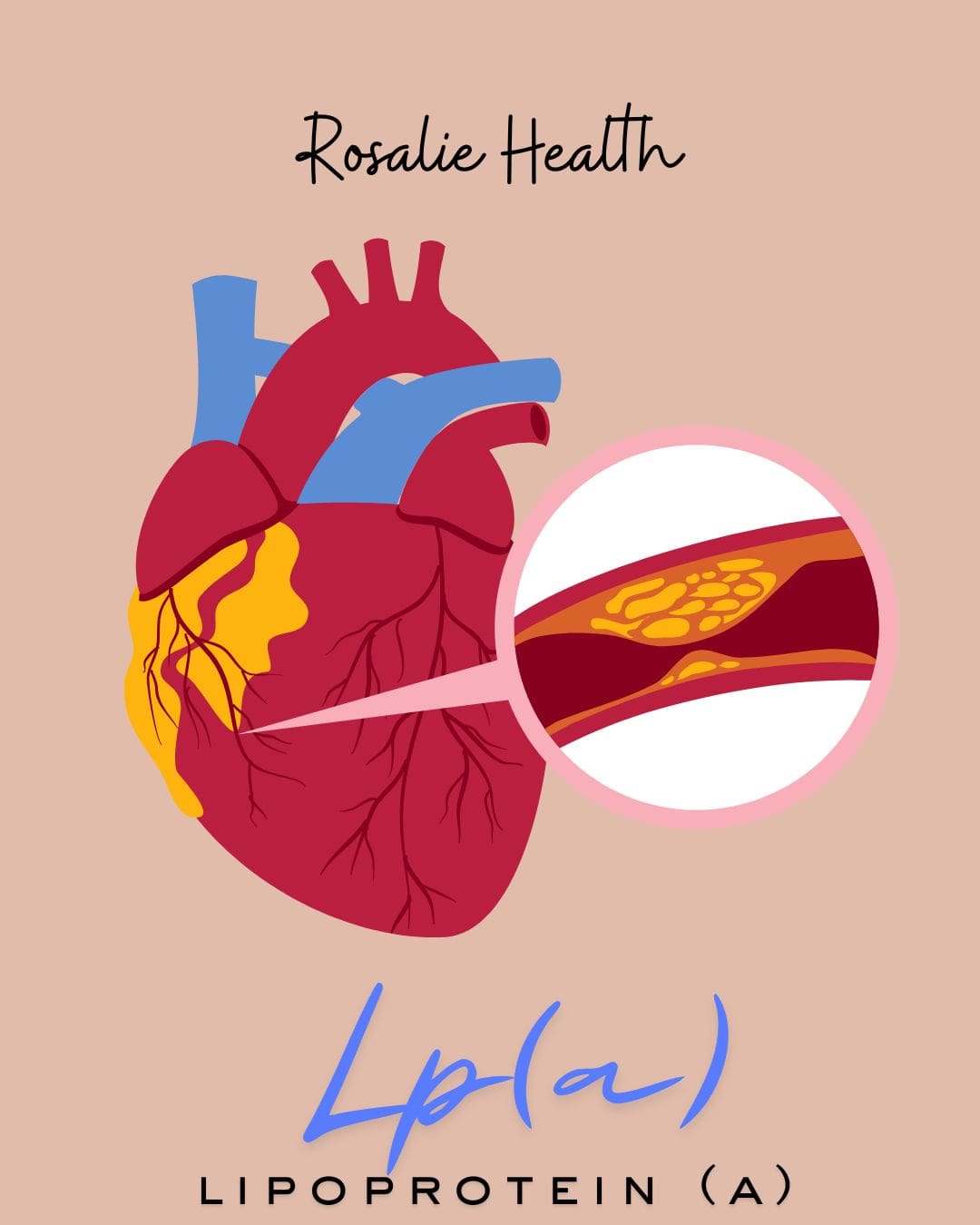
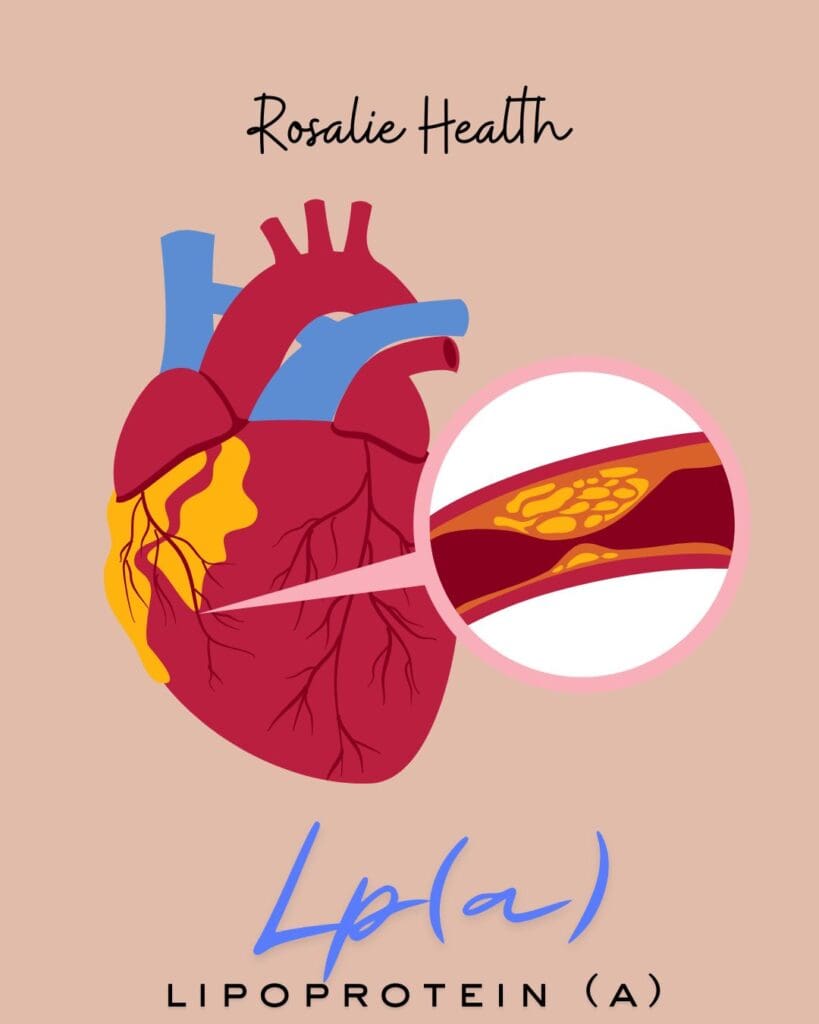
Lp(a) — The Cholesterol Marker You’ve Probably Never Had Checked (But Should)

Posted In
April 29, 2026
Posted On
Keywords: Lp(a) cardiovascular risk, lipoprotein a test, what is Lp(a), heart disease risk factors women
You’ve had your cholesterol checked. LDL? Fine. HDL? Decent. Triglycerides? Your doctor smiled. And yet something in you wonders: is that really the whole story?
If nobody has measured your Lp(a), the answer might be no.
What Is Lp(a)?
Lp(a) — pronounced “L-P-little-a” — stands for lipoprotein(a). It’s a type of LDL particle with an extra sticky protein called apolipoprotein(a) attached. That stickiness makes Lp(a) significantly more likely to promote plaque buildup in the arteries, trigger blood clot formation, and drive inflammation in vessel walls — independent of your other cholesterol numbers.¹
In plain English: you can have perfectly “normal” LDL and still carry elevated cardiovascular risk if your Lp(a) is high. And most standard lipid panels don’t even check it.
What Does Lp(a) Tell Us?
The American Heart Association (AHA) and the European Atherosclerosis Society (EAS) both recognize elevated Lp(a) as an independent risk factor for cardiovascular disease — meaning it raises your risk even when everything else looks good on paper.²
Specifically, elevated Lp(a) is associated with:
- Increased risk of heart attack and stroke
- Accelerated coronary artery disease
- Aortic valve stenosis
- Recurrent cardiovascular events in those with established disease
Optimal Lp(a) levels are generally below 30 mg/dL (or <75 nmol/L). Levels above 50 mg/dL are considered high risk and warrant proactive cardiovascular monitoring.
Here’s the Kicker: It’s Mostly Genetic
Unlike LDL cholesterol, which is heavily influenced by diet and lifestyle, Lp(a) levels are approximately 70–90% determined by genetics, according to research published in the New England Journal of Medicine.³
This means no amount of oat bran or cardio will dramatically lower it. And it also means: this is not your fault. If your Lp(a) is elevated, you inherited it — and the most empowering thing you can do is simply know your number so you can act accordingly.
Who Should Get Tested?
The 2019 AHA/ACC Cardiovascular Risk Guidelines recommend Lp(a) testing for:
- Anyone with a personal or family history of premature cardiovascular disease
- Women, particularly post-menopause (estrogen helps regulate Lp(a))
- Those with borderline cardiovascular risk who need more clarity
- Anyone with unexplained cardiovascular events
Because Lp(a) is so strongly genetic, it typically only needs to be measured once in a lifetime — but that once is genuinely important.
What Can You Do About It?
While Lp(a) itself is difficult to lower through lifestyle alone, knowing your number lets us get much more intentional about your overall cardiovascular health. A personalized approach may include aggressive management of modifiable risk factors (blood pressure, inflammation, insulin resistance), targeted nutritional support for vascular health (omega-3s, niacin, CoQ10), earlier cardiovascular screening, and awareness of emerging RNA-based therapies currently in clinical trials.⁴
You can’t change your genes. But you can make sure they don’t catch you off guard.
Book a Cardiovascular Consultation at Rosalie Health → www.RosalieHealth.com
References
1. Tsimikas S. A Test in Context: Lipoprotein(a). J Am Coll Cardiol. 2017;69(6):692-711. https://doi.org/10.1016/j.jacc.2016.11.042
2. Nordestgaard BG, et al. Lipoprotein(a) as a cardiovascular risk factor: current status. Eur Heart J. 2010;31(23):2844-2853. https://doi.org/10.1093/eurheartj/ehq386
3. Clarke R, et al. Genetic variants associated with Lp(a) lipoprotein level and coronary disease. N Engl J Med. 2009;361(26):2518-2528. https://doi.org/10.1056/NEJMoa0902604
4. Koren MJ, et al. Acknowledgment of Lp(a)-Lowering Therapies in Current Guidelines. J Am Coll Cardiol. 2022;79(11):1107-1117.
Rosalie Health | www.RosalieHealth.com | 610-427-5772 | West Chester & Ardmore, PA | Virtual visits available
Pin
Share
Leave a Reply Cancel reply
Previous Story
next Story
© 2026 Rosalie Health LLC. Site by Alexa Lucky Creative
@rosaliehealth
Join Me on Insta
A simple, free guide to help you make sense of your thyroid lab results.
Your Thyroid
Lab Guide
Free Guide
233 E. Lancaster Ave, Suite 103
Ardmore, PA 19003
Hours: By appointment only
ariella@rosaliehealth.com
Call or text: (610) 427-5772
780 E. Market Street, Suite 280
West Chester, PA 19382